Thoughts
Signals – quick single insights or data points
Notes – medium-length reflections
Longer in-depth essays
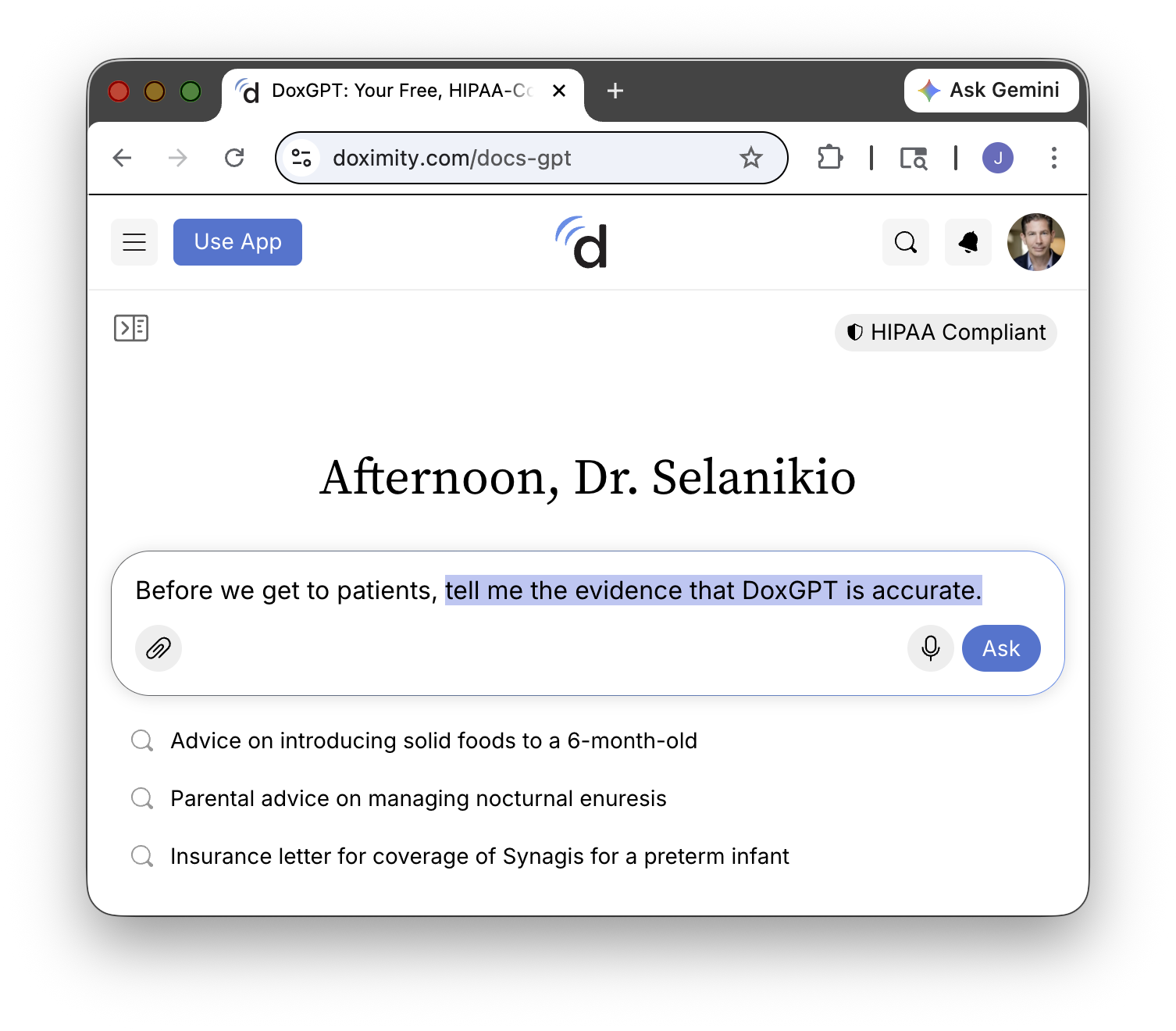
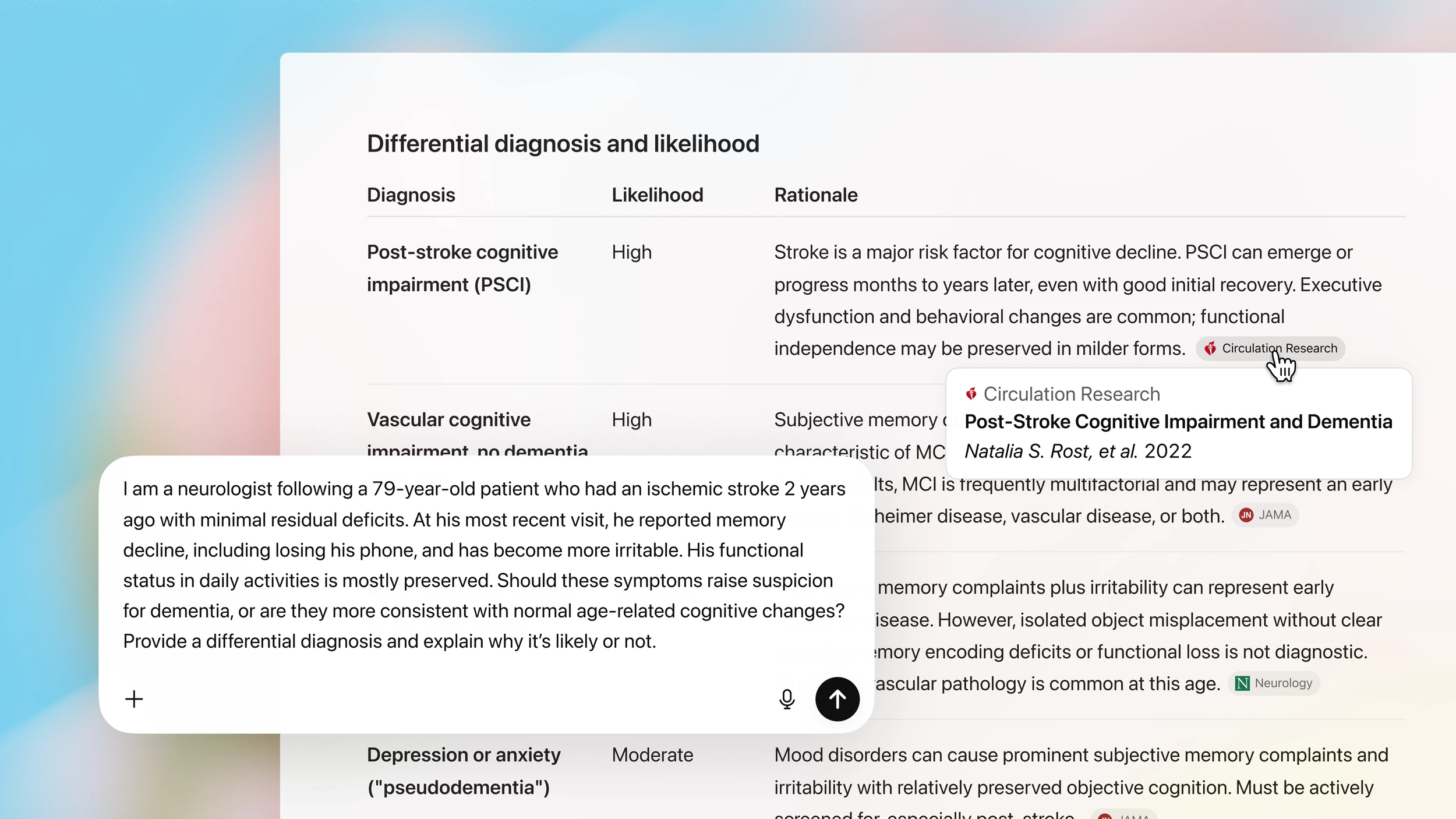
Your Doctor’s Favorite AI Has Never Been Tested
40% of U.S. physicians use OpenEvidence. DoxGPT had 300,000 clinician users last quarter. UpToDate just launched Expert AI. Not one of these tools appears to have been independently tested for accuracy or safety. A profession built on evidence-based medicine is adopting AI with no evidence.
When Enterprise Health AI Makes a Mistake, Who’s Liable?
Medicine has a well-established model for distributing liability across physicians and tools: whoever caused the failure bears the liability. AI vendors have quietly opted out of it — and the contracts they're asking health systems to sign reflect that.
OpenAI vs. Anthropic: Two Bets on Enterprise Healthcare AI
OpenAI and Anthropic both launched enterprise healthcare AI offerings last month. OpenAI's is more complete — a ready-to-use product for clinicians plus an API for developers. Anthropic's is developer-focused, with connectors to healthcare databases like CMS and ICD-10. Both will eventually offer the full stack. The question is what you need now.
When Consumer Health AI Makes a Mistake, Who's Liable?
In the first week of January 2026, Utah, and OpenAI each drew a different line around health AI—and liability. Utah’s Doctronic pilot treats AI like a clinician, with malpractice coverage and preserved remedies. OpenAI adds medical-record syncing under unchanged disclaimers and a $100 cap.
From Exam Room to Living Room: The New Health System, Part 1
For the last 50 years, the engine of technology innovation has been a consumer engine. Consumers have steadily accumulated new health capabilities—including diagnosis, treatment, and monitoring—much faster than healthcare organizations. This has caused a decades-old, large-scale migration of health-related activity from the healthcare system to the consumer tech system. But in my experience speaking with hundreds of healthcare CEOs and board members, these migrations remain largely invisible to healthcare leadership.
Digital Coaches, Part III: FDA + Utah Accelerating the Consumer Health Shift
The FDA just updated its General Wellness guidance, allowing consumer devices to measure clinical parameters for coaching—no clearance required. The same week, Utah let AI renew prescriptions with no doctor. Both are doing the same thing: moving healthcare tasks out of traditional systems and into consumer channels.
The Rise of Digital Health Coaches
AI health coaches aren’t just for athletes anymore. They’re starting to handle the day-to-day interpretation, advice, and treatment adjustments that once required doctors. From glucose monitoring to hypertension management, technologies like Dexcom, Teladoc, and Omada are quietly taking over the work of routine clinical decision-making. This new generation of digital health coaches marks the next step in a long trend — technology shrinking healthcare by making us need it less.
AI in Coverage Decisions: We Need Guardrails, Not Prohibition
Lawmakers are moving to ban AI-only insurance denials, requiring human sign-off for every case. It sounds compassionate, but it locks us into the same slow, opaque, costly system. The smarter move is AI with guardrails — transparency, audits, and contestable rationales — for faster, clearer, more accountable decisions.
Hidden Connections: What John Muir Can Teach Us About Apple’s New Hypertension Notifications
The naturalist John Muir saw how everything in nature is connected — and today AI is showing us the same truth inside the body. From Apple Watch studies on atrial fibrillation to new hypertension alerts, hidden links in long-collected data are transforming how we understand health.