Thoughts
Signals: AI is Killing 14 Million Clinic Visits — Per Month
Gallup and West Health just gave us some solid data on demand migration.
In a nationally representative survey of 5,500 U.S. adults released April 15, 14% said the AI-generated advice led them to skip a provider visit in the past 30 days. Projected to the adult population, that's roughly 14 million missed appointments in a single month.
Notes: the Prescription You Can’t See
Eighteen percent of AI chatbot users have adjusted a medication based on a chatbot conversation. No doctor, no clinical oversight, no documentation anywhere in the healthcare system. The prescribed regimen and the actual regimen are diverging moore and more, via a channel that is invisible to healthcare.
The $50B Measurement Blind Spot in Healthcare Strategy
I speak with at least 100 healthcare leaders each year. They track everything — length of stay, readmissions, OR utilization, revenue cycle velocity. The one thing they're not tracking at all? The demand leaving the system entirely. And a Harvard finding that should have set off alarms six years ago has gone almost completely unnoticed.
A Podcast with Scott Becker of Becker’s Hospital Review
Happy to discuss healthcare growth, primary care’s decline, consumer health tech, and self-driving cars with the very well-informed Scott Becker, in this episode of Becker’s Healthcare Podcast.
The ATM, the iPhone, and Your Doctor's Office
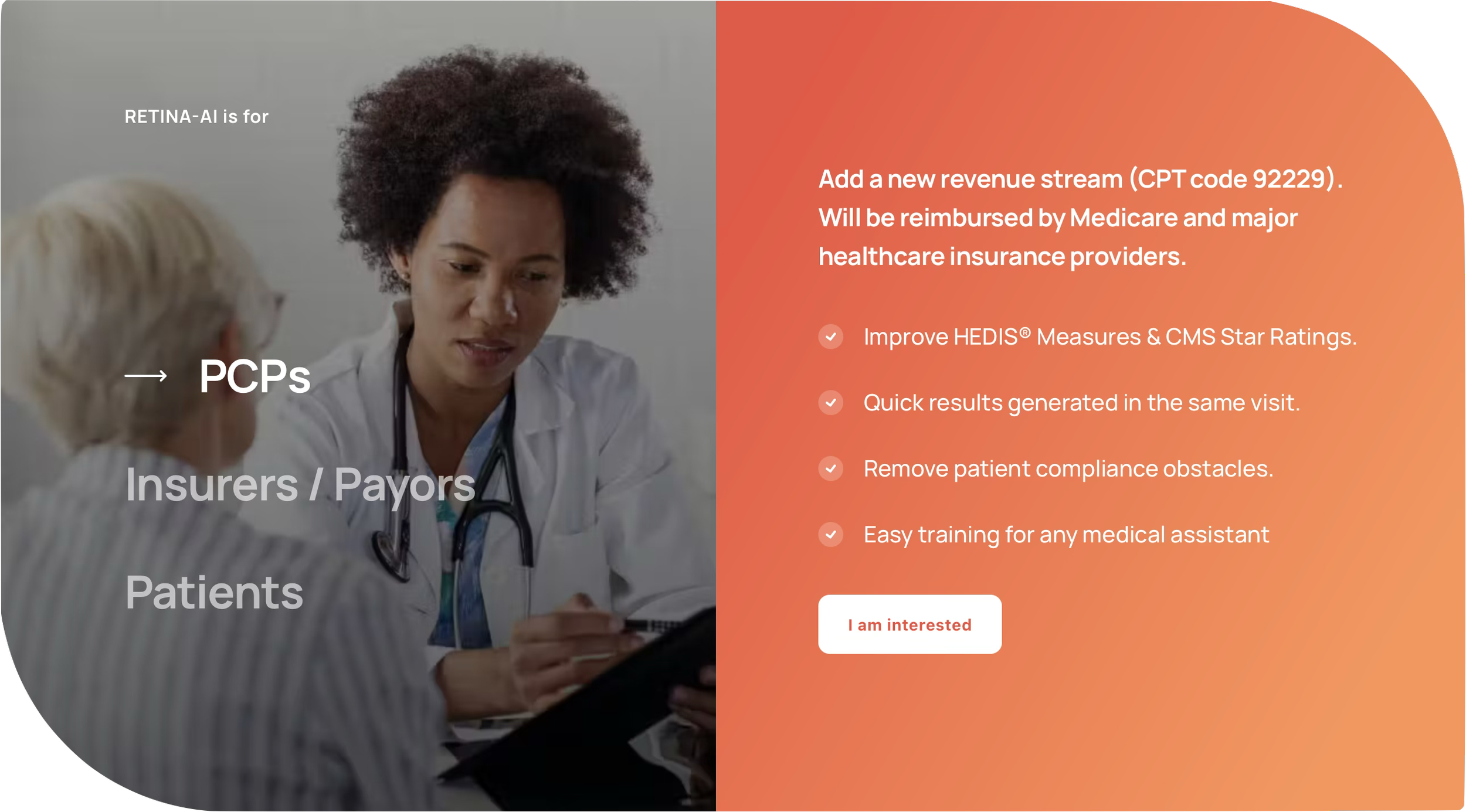
Clinical AI can make doctors more efficient and reduce burnout. But wearables, GLP-1 drugs, direct-to-consumer labs, and AI health assistants are doing something far more radical: they’re making many traditional doctor visits unnecessary. The real disruption in healthcare is already happening outside the exam room.
Signals: Was the Diagnosis Already in the Chart?
Stanford researchers gave AI radiology test questions without the images. The AI aced them anyway. Most people think that's a knock against AI. I think it's telling us something about the images.
Signals: Geoff Hinton Not Wrong After All?
Hospital CEOs are saying they’re ready to replace radiologists with AI for first reads. The radiology community has spent nine years saying that would never happen.
They can’t both be right.
Your Doctor’s Favorite AI Has Never Been Tested
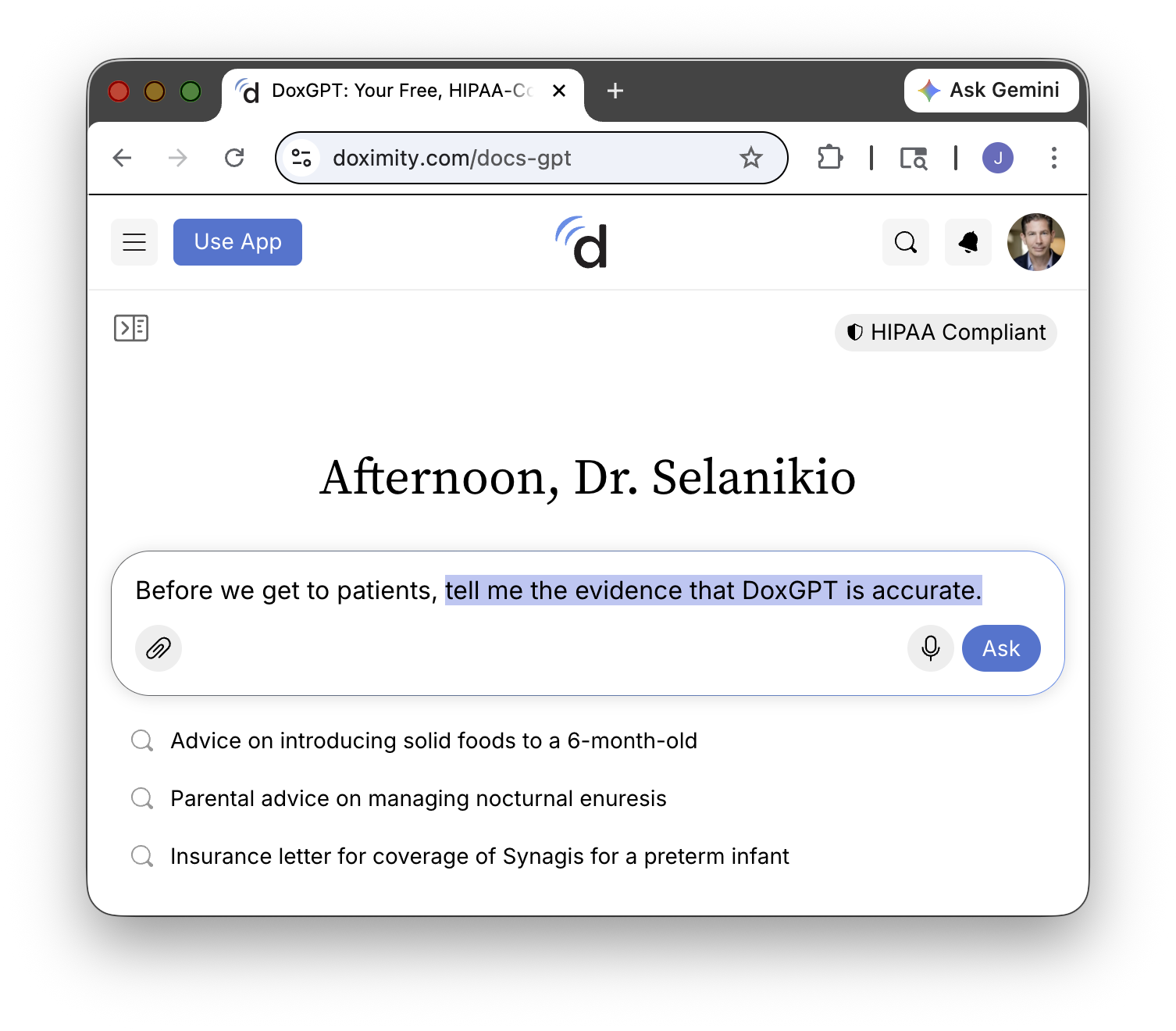
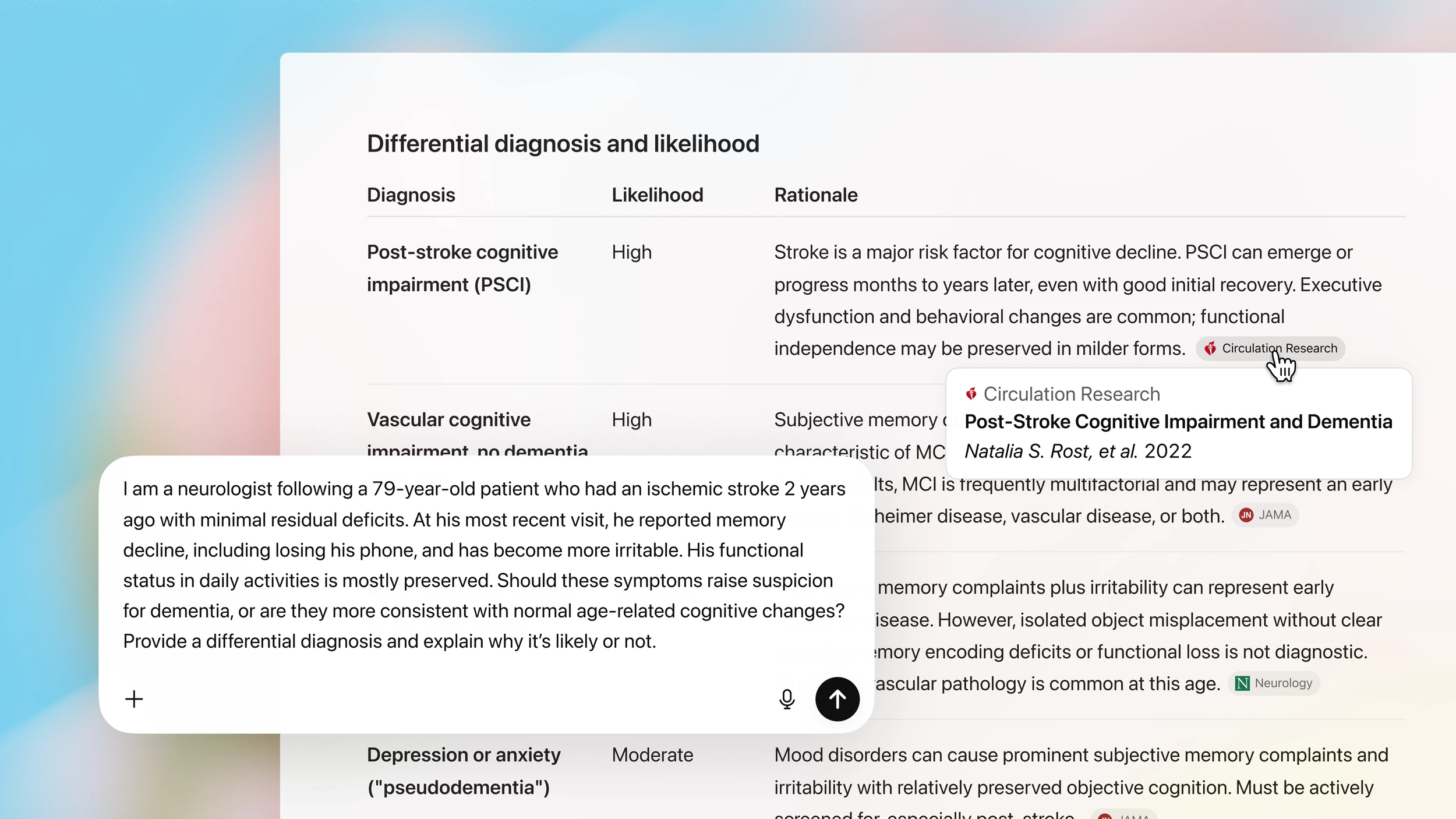
40% of U.S. physicians use OpenEvidence. DoxGPT had 300,000 clinician users last quarter. UpToDate just launched Expert AI. Not one of these tools appears to have been independently tested for accuracy or safety. A profession built on evidence-based medicine is adopting AI with no evidence.
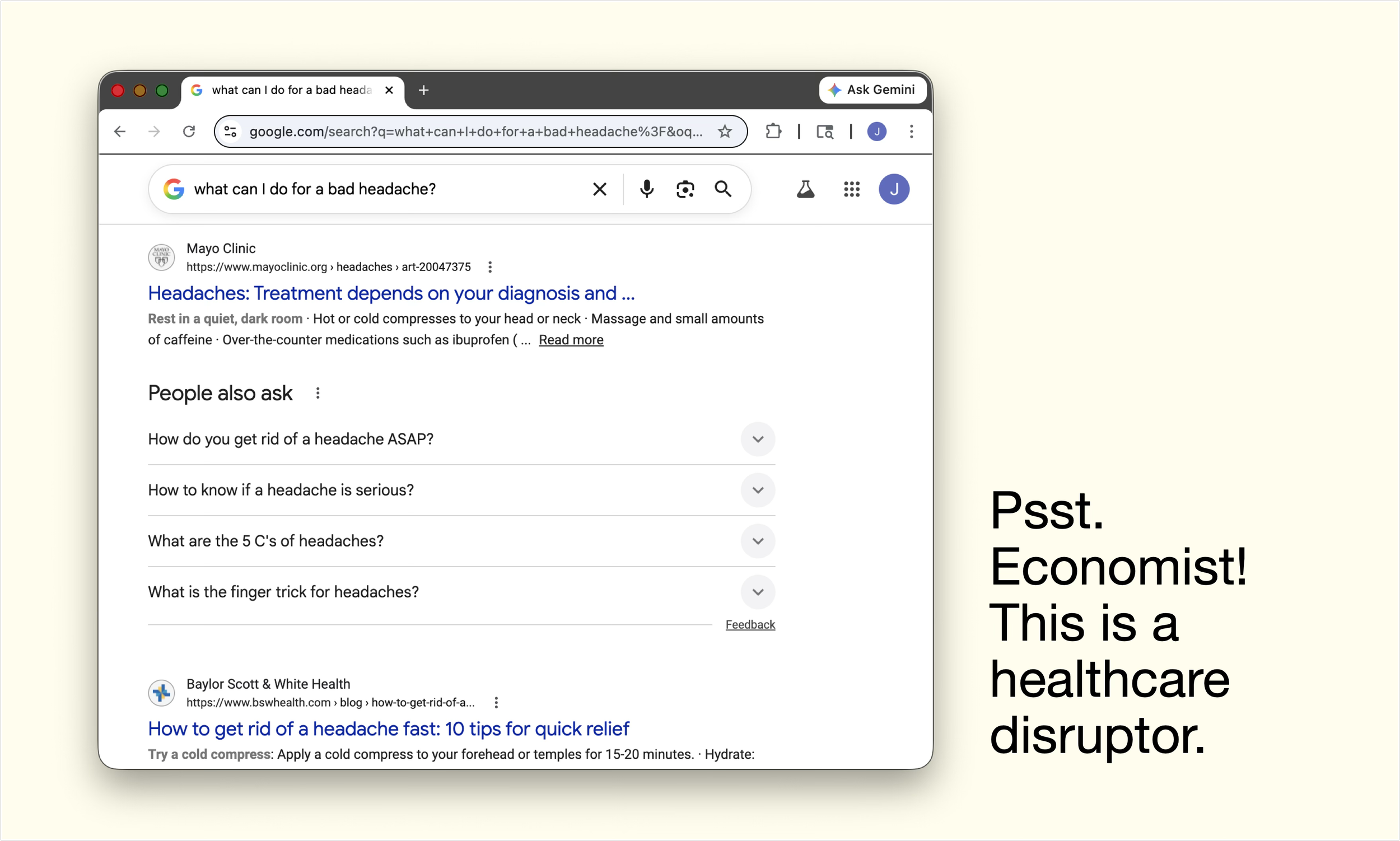
The Economist Wrote About Healthcare Disruption — But Missed the Disruption
The Economist says healthcare has "proved resistant to treatment from disrupters." If that's true, why has per capita spending growth been falling for fifty years? Why have primary care visits dropped 24%?
Because the Economist, and the healthcare system, don't count disruption that doesn't call itself healthcare.
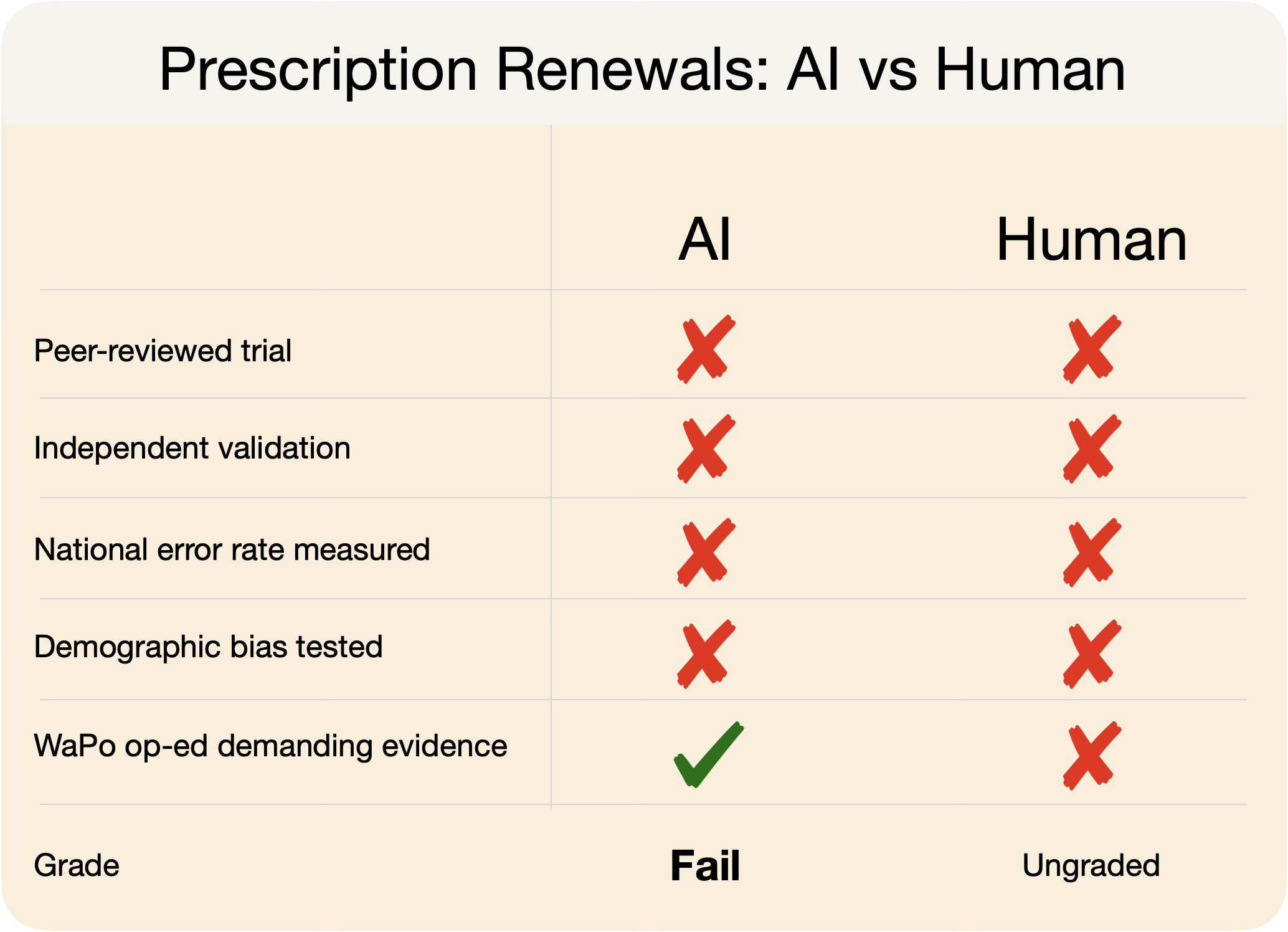
We Want to Grade the AI. Did We Grade the Doctor?
A Washington Post op-ed argues that Utah's AI prescription renewal pilot rests on thin evidence. Fair. But the human renewal process it's replacing has never been rigorously validated either. We're applying a standard to AI that we've never applied to the human baseline.
When Enterprise Health AI Makes a Mistake, Who’s Liable?
Medicine has a well-established model for distributing liability across physicians and tools: whoever caused the failure bears the liability. AI vendors have quietly opted out of it — and the contracts they're asking health systems to sign reflect that.
OpenAI vs. Anthropic: Two Bets on Enterprise Healthcare AI
OpenAI and Anthropic both launched enterprise healthcare AI offerings last month. OpenAI's is more complete — a ready-to-use product for clinicians plus an API for developers. Anthropic's is developer-focused, with connectors to healthcare databases like CMS and ICD-10. Both will eventually offer the full stack. The question is what you need now.
When Consumer Health AI Makes a Mistake, Who's Liable?
In the first week of January 2026, Utah, and OpenAI each drew a different line around health AI—and liability. Utah’s Doctronic pilot treats AI like a clinician, with malpractice coverage and preserved remedies. OpenAI adds medical-record syncing under unchanged disclaimers and a $100 cap.
The Continuous "Dr. You": OpenClaw and the Future of Personal Health Management
Current AI health tools share the same flaw as traditional healthcare: they're episodic, not continuous. OpenClaw — a nerdy new tool that’s shot to 2 million users in nothing flat — shows us what comes next: AI assistants that monitor your health 24/7, cross-reference data sources, and act on your behalf without being asked.
From Exam Room to Living Room: The New Health System, Part 1
For the last 50 years, the engine of technology innovation has been a consumer engine. Consumers have steadily accumulated new health capabilities—including diagnosis, treatment, and monitoring—much faster than healthcare organizations. This has caused a decades-old, large-scale migration of health-related activity from the healthcare system to the consumer tech system. But in my experience speaking with hundreds of healthcare CEOs and board members, these migrations remain largely invisible to healthcare leadership.
Digital Coaches, Part III: FDA + Utah Accelerating the Consumer Health Shift
The FDA just updated its General Wellness guidance, allowing consumer devices to measure clinical parameters for coaching—no clearance required. The same week, Utah let AI renew prescriptions with no doctor. Both are doing the same thing: moving healthcare tasks out of traditional systems and into consumer channels.
Bad Timing: Will GLP-1s Bankrupt Health Insurance Before They Save It?
Blue Cross Blue Shield of Massachusetts just posted a $400 million loss—the worst in their history. The culprit? GLP-1 medications that could eventually save insurers billions. The costs hit today, the savings arrive years later, and health systems are caught in the middle.
The First Healthcare Demand Shock of the 21st Century
GLP-1 medications may do far more than treat diabetes or reduce weight. If they substantially cut obesity and metabolic disease, they could trigger the first large-scale decline in healthcare demand seen in the modern era. This piece explores how earlier demand shocks reshaped medicine, why GLP-1s pose a similar challenge for chronic-disease–based service lines, and what hospitals must do now to prepare for a world with fewer cardiometabolic patients.
The New York Times Got Smaller — Healthcare Is Next
The New York Times built one of the best digital products in media—yet its real revenue and profit have fallen by more than half. That’s what disruption actually looks like: the work moves elsewhere while the industry shrinks. Healthcare is now entering the same pattern, driven by consumer tech, GLP-1s, and safer mobility. We’re heading toward better health—and a smaller healthcare system.
Digital Coaches, Part II: Prevention’s New Business Model
Digital coaches are taking prevention where healthcare and public health can’t reach — into daily life. Activity trackers like Apple Watch, Fitbit, and Garmin now deliver personalized, continuous feedback at global scale, turning prevention into a business that keeps people healthier — and needing healthcare less.